For years a top 10 long-term disability carrier struggled to make significant improvements in its core claims (own occ) processing. Although the carrier had made incremental process and technology reforms over the years, their key metric for success – the number of claims remaining open one month after change of definition – nevertheless remained stubbornly high. This metric is of critical importance because any claim that has been positively impacted prior to change of definition is either a successful RTW, a claim denial, an early move to low-touch handling, or a transition to any occ or settlement. The remaining claims are those whose status is uncertain, and whose claimants are still in need of help. While there will always be some difficult claims of this nature, the fewer of these that remain, the better job the organization is doing of getting the right resources to their claimants as quickly as possible. This in turn results in faster claim closures.
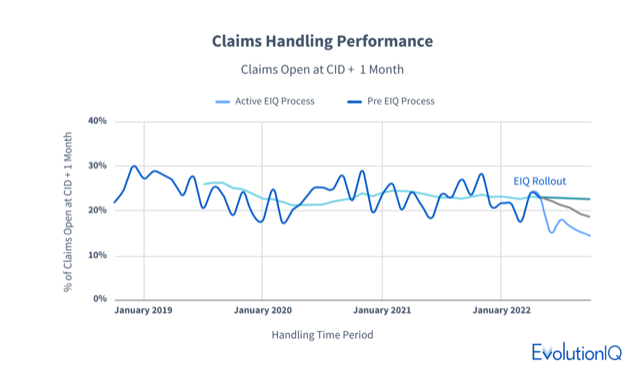
As the chart below shows, for years this metric at this carrier hovered around 23% of claims. However, once they started using EvolutionIQ Claims Guidance, that percentage trended sharply downward, with open claims at 14.4% in October 2022.
Naturally, this increase in claim closures meant an overall decrease in claim durations. In fact, claim durations declined by 30 days. Reducing claim durations saved the organization more than $4 million in net benefit payments alone. Based on their current performance, the carrier is projected to reduce durations by an additional 15 days in 2023, making a total reduction of 45 fewer days per claim vs. the non-EvolutionIQ assisted performance. And all of this took place within 6 months of the initial deployment of EvolutionIQ Claims Guidance.
The end result — increased RTW, decreased open claims at change of definition plus one month, and reduced overall claim durations put money directly to the bottom line. Upgrade your Core claims processing with EvolutionIQ Claims Guidance.